PSA Blood Test
€45,00
Free Shipping to
Prostate-specific antigen (PSA) is a protein produced by the prostate and is released into the blood in small amounts. When there is a problem with the prostate, such as prostate cancer, PSA levels in the blood can rise. PSA testing can help identify prostate cancer in an earlier stage. This home PSA Test can detect high levels of PSA that may be indicative of prostate cancer or inflammation.
Test mode: Finger prick Dry Blood Spot test
What do we test for?
About Prostate-Specific Antigen
Prostate-Specific Antigen (PSA) is a protein produced by the cells of the prostate gland in males. The main function of PSA is to liquefy the semen that carries sperm during ejaculation. A small amount of PSA is normally present in the blood of men, but elevated levels can be an indicator of various prostate-related conditions. The most well-known use of PSA is as a screening test for prostate cancer. However, it's important to note that elevated PSA levels do not necessarily indicate prostate cancer. Other non-cancerous conditions, such as prostatitis (inflammation of the prostate) or benign prostatic hyperplasia (enlargement of the prostate), can also cause increased PSA levels.
€45,00
Free Shipping to
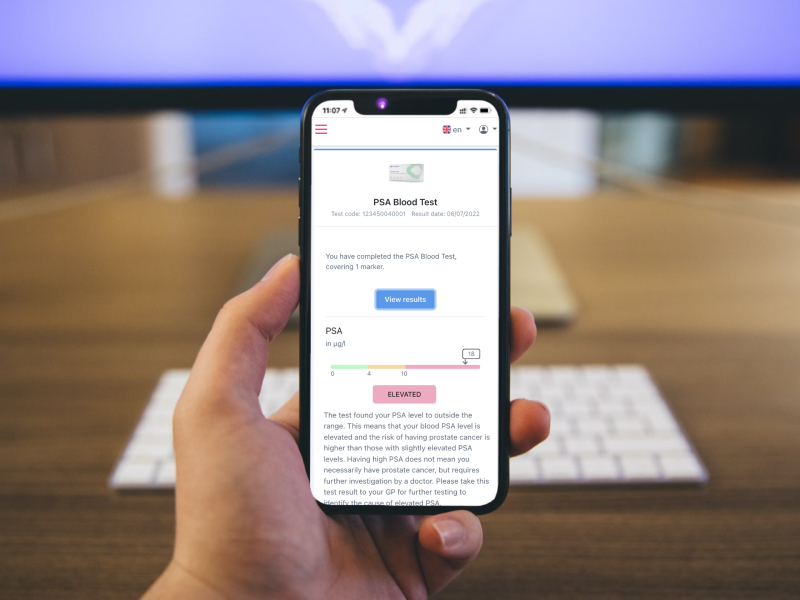
How does a PSA test work?
The PSA test is a blood test that can be performed at home. A small blood sample is collected via a finger-prick and then sent to our laboratory for analysis. Homed-IQ’s health tests come with everything you need to successfully take a blood sample at home. Simply activate your test and follow the provided instructions to successfully collect the sample and then send it to our certified laboratory using the prepaid shipping label. The results will be available within a few days.
Who should use this test?
Men between the ages of 50 and 74 with an average risk of prostate cancer may consider doing a PSA test. If prostate cancer runs in your family or you are considered to be at high risk, you may consider testing before age 50. Before performing this test it is important to understand the risks and benefits. Please read “Risks and Benefits of Testing” before making the decision to perform this test. If you are unsure whether PSA testing would be appropriate for you, please contact your GP.
PSA
Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland in males. The main function of PSA is to liquefy the semen that carries sperm during ejaculation. A small amount of PSA is normally present in the blood of men, but elevated levels can be an indicator of various prostate-related conditions. The most well-known use of PSA is as a screening test for prostate cancer. However, it’s important to note that elevated PSA levels do not necessarily indicate prostate cancer. Other non-cancerous conditions, such as prostatitis (inflammation of the prostate) or benign prostatic hyperplasia (enlargement of the prostate), can also cause increased PSA levels.
Weighing the risks and benefits
The PSA test is a screening test for prostate cancer. Screening tests aim to find cancer in people before they have symptoms. Screening can help find cancers at an earlier stage, when they are possibly easier to treat. If prostate cancer is found early as a result of screening, it could seem like PSA testing would always be a good idea. However, it is important to understand the risks and benefits of testing to decide if it is right for you. The choice to do a PSA test is an individual decision that should be made after understanding the risks and benefits of testing.
Benefits of PSA testing:
- Can detect prostate cancer before you have any symptoms
- Can detect a fast growing cancer at an early stage, before it spreads to other parts of the body and becomes difficult to treat
Doctors are still studying whether PSA testing lowers the risk of death from prostate cancer. Current study results on the benefits of screening are conflicting, which is why the choice to do a PSA test should be a personal one.
Results from a large European study of prostate cancer screening found that men who had prostate-specific antigen (PSA) testing had a 20 percent lower chance of dying from prostate cancer after 13 years, compared with men who did not have prostate cancer screening (Hugosson et al., 2019). However, the study also showed that 781 men would need to prevent one death from prostate cancer (Schröder et al., 2014). This means that testing the general population involves many men getting tested, and a very small number benefitting.
Risks of PSA testing:
Inaccurate test results
There is a chance of a false positive test result with all screening tests. This means that your PSA level is elevated but no cancer is present. A false-positive test result may create anxiety for you and your family, or lead to additional invasive medical procedures with their own side effects, such as a prostate biopsy. As multiple factors can cause PSA levels to rise, false positive PSA test results are common; approximately 25% of people who have a prostate biopsy due to an elevated PSA level are found to have prostate cancer after biopsy (Lopez-Corona et al., 2007).
A false negative test result means that the PSA level is found to be normal when prostate cancer is present. Approximately 15% of individiuals with prostate cancer do not have elevated PSA levels (Prostate Cancer UK, 2021). A false negative test result may provide false reassurance that no cancer is present. If you are experiencing prostate-related symptoms despite a normal PSA level, always contact your GP.
Overdiagnosis and overtreatment
Overdiagnosis means diagnosing a condition that would never pose a threat to your health or life. Overdiagnosis can lead to treatments that are not necessary and have their own side effects, known as overtreatment. This can result in an individual sustaining harms with no benefits from screening for a disease. Research estimates 23% 43% of prostate cancers that are diagnosed with PSA testing may never need to be treated and will not affect a man’s life expectancy (Sandhu & Andriole, 2012). This means that many men die “with” prostate cancer, rather than “from” prostate cancer. However, most men who are diagnosed with prostate cancer understandably want to pursue treatment. Unnecessary testing and treatment can cause side effects such as incontinence, pain, and erectile dysfunction.
An elevated PSA level alone does not cause symptoms. However, if you are experiencing symptoms that indicate problems with the prostate, you may consider doing a PSA test. Potential symptoms include:
- Difficulty starting to urinate
- Urinary incontinence
- Slow urine stream
- Frequent urination
- The feeling that your bladder is not completely empty after urinating
- Pain when urinating
- Pain when ejaculating
- Blood in the urine or semen
- Problems getting or maintaining an erection
What do the test results mean?
This test measures the PSA level in your blood. The results of this test cannot specifically tell you if you have prostate cancer.
There is no specific normal or abnormal PSA level in the blood.
- Generally, a PSA level of less than 4.0 ng/mL is considered normal. For dry blood spot testing methods, a normal PSA level is less than 4.4 ng/mL.
- A PSA level between 4.4 and 10.0 ng/mL is considered to be the “borderline range” in which the risk of prostate cancer is higher.
- A PSA level higher than 10.0 ng/mL indicates a greater than 50% chance of prostate cancer.
Please note: While a PSA test can be used to help detect prostate cancer, it is not perfect. Some cases of prostate cancer do not cause high PSA. It is also possible to have high PSA and not have prostate cancer. If you are experiencing symptoms consistent with prostate cancer, always contact your GP for further examination regardless of PSA level.
Factors such as age, prostate enlargement/inflammation, cycling, and recent ejaculation can also increase PSA levels. Furthermore, certain drugs can lower PSA levels. Recent research has suggested the following lower PSA limits for each age group:
40 – 49 years : 2.50 µg/l
50 – 59 years : 3.50 µg/l
60 – 69 years : 4.50 µg/l
70 – 79 years : 6.50 µg/l
In combination with your PSA test result, ask your GP about the possibility of a prostate exam to confirm there are no abnormalities.
What should I do if my test result shows elevated PSA?
If your blood PSA is higher than normal, it doesn’t always mean you have prostate cancer. Many men with elevated PSA do not have cancer. Please take your test result to your doctor for further investigation. Further testing may include:
- Waiting a while and taking a second PSA test to see if levels have changed
- Getting another type of PSA test (such as free PSA) to check if a prostate biopsy is needed
- Physical prostate exam
- Prostate biopsy
Frequently asked questions
Are there any other tests that can indicate prostate cancer?
What is a normal PSA value?
- Generally, a PSA level of less than 4.0 ng/mL is considered normal. For dry blood spot testing methods, a normal PSA level is less than 4.4 ng/mL.
- A PSA level between 4.0 and 10.0 ng/mL is considered to be the “borderline range” in which risk of prostate cancer is higher.
- A PSA level higher than 10.0 ng/mL indicates a greater than 50% chance of prostate cancer.
How quickly can PSA levels rise?
What factors affect PSA level in the blood?
- Older age
- Prostate enlargement or other conditions
- Urinary tract infection
- Vigorous exercise, particularly bike riding
- Recent ejaculation
- NSAIDs
- Statins
Do you need to fast before a PSA test?
How often should you check your PSA level?
- Men who choose to be tested who have a PSA of less than 2.5 ng/mL may only need to be retested every 2 years.
- Screening should be done yearly for men whose PSA level is 2.5 ng/mL or higher.