It’s not often talked about, but your bowel movements can say a lot about your health. Not only are colour and consistency important factors, but smell and how often you go to the toilet are also relevant cornerstones by which you can gauge the state of your health. But what exactly is a healthy bowel movement? Is diarrhea dangerous? Or is blood in the stool always a sign of colon cancer? And how often should one actually visit the toilet on average? While our article “What can be detected in a stool sample?” focused on explaining diseases and bacteria that can be detected in a stool sample, in this article we will share characteristics of both healthy and unhealthy stool.
When is a bowel movement considered healthy?
In general, stool is healthy when it is light to dark brown in colour, neither runny nor hard, and smells bad but is not acrid or putrid. But why are bowel movements important? Your body and its digestive tract excretes numerous unusable food residues via the stool. In addition to these food residues, stool also contains other waste products from metabolism and digestion. These include:
- Breakdown products of hemoglobin – these give your stool its characteristic colour
- Water
- Mucus
- Digestive liquids
- Dead microorganisms from your intestinal flora
- Cells from the intestinal mucosa, which are regularly shed
If your bowel movements smell stronger than normal or are liquid, you don’t have to worry immediately as certain foods can affect bowel movements. Products containing sugar, dairy products, and certain vegetables such as cabbage can cause your stool to smell particularly strong and unpleasant due to their comparatively high sulphur content.
Colour of stool
In addition to an unpleasant smell, certain foods can also cause your stool to differ from the normal brown colour. It is not uncommon for someone to become very concerned because their stool is reddish in colour. However, the cause is often the consumption of foods containing beetroot or red food colouring. Sometimes, however, medication can also cause your stool to turn reddish or pink. If there is blood in your stool, you should contact your family doctor. On one hand, blood in the stool can “only” be hemorrhoids, but it can also indicate abnormal growths in the colon or colon cancer.
Many green vegetables, such as kale and spinach, can also cause your stools to be greenish in colour. However, greenish diarrhea can be an indication of a gastrointestinal infection and not just the result of diet.
Yellowish or orange-colored stools can often be caused by yellow/orange foods such as carrots or squash. In addition to food, medications such as antibiotics can also cause a yellowish/orange colour in stool. However, yellow stools can also indicate problems with the pancreas, gallstones or gluten intolerance (celiac disease). If your stool has a pungent odour and is difficult to flush, you are considered to have fatty stool.
Black and white stool is also possible. While black stool can also be caused by charcoal tablets and iron supplements, among other things, white stool usually indicates problems with the bile.
Important: While black stool can be caused by charcoal tablets and iron supplements, it can also indicate upper digestive tract bleeding. Often the amount of blood in the stool is not enough to turn the stool red or black, which can lead to bleeding around the intestinal tract going unnoticed for extended periods of time, which makes treatment more difficult in an emergency. It is therefore highly advisable to consider performing regular colon cancer screening tests from the age of 50.
Consistency of stool
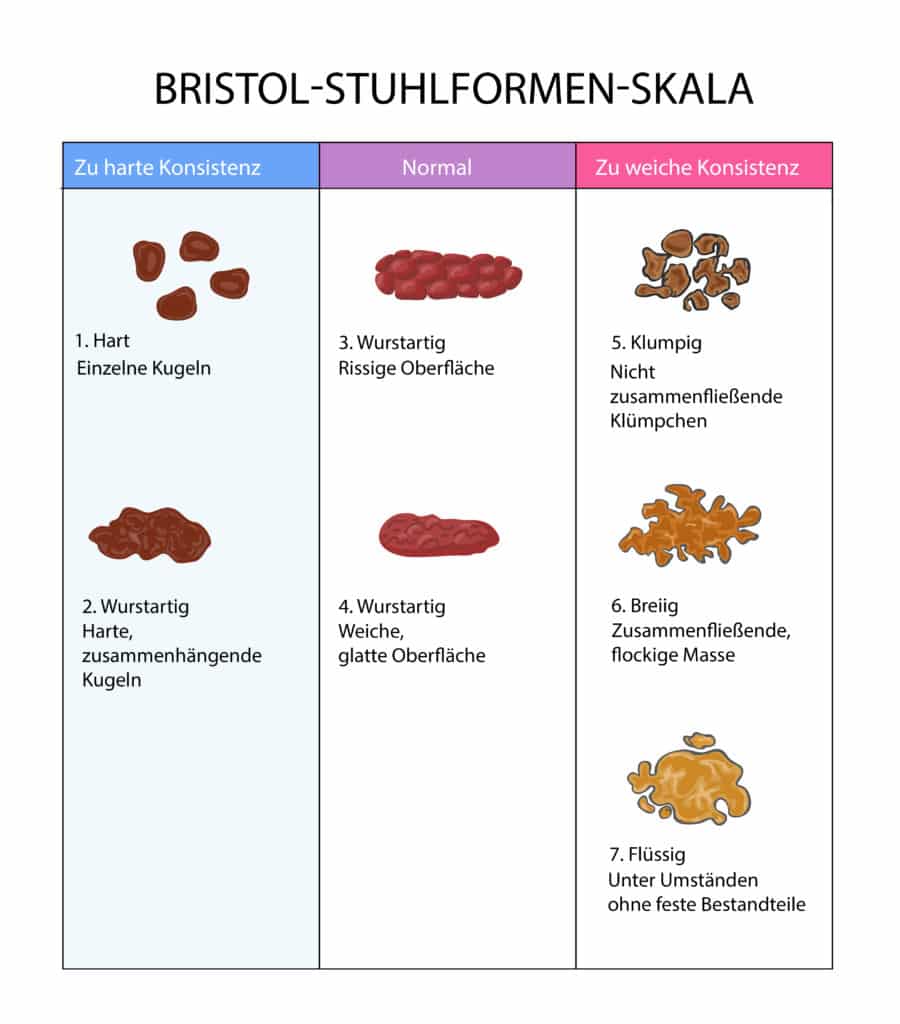
As mentioned at the beginning, stool can come in a variety of shapes and colors. Thanks to science, there is a proven scale for classifying bowel movements. The Bristol Stool Form Scale was developed in 1997 by researchers at the British University of Bristol. Over time, several studies have confirmed the reliability of the scale, which is why this scale is still used by doctors today, more than 25 years later.
The consistency of stool can be divided into seven types, which in turn are divided into three categories – too soft consistency, normal consistency and too hard consistency. Stool consistency can be broken down into the following types:
Frequency of bowel movements
Now that we’ve learned about colour and consistency, how often do you have “normal” bowel movements? There is no general answer to this question, as it varies from person to person. In principle, however, you don’t need to immediately worry if you haven’t had a bowel movement in three days – you are not necessarily suffering from an intestinal obstruction. Generally, it is said that having a bowel movement once a day is ideal. However, this is only a guide and does not mean that you should worry if you deviate from it. According to an American study on the frequency and timing of bowel movements, only 40% of the American population meets this standard. 95.5% of the participants fall under the so-called 3-3 rule. This rule states that human bowel movements vary between three times a day and three times a week.
The frequency of bowel movements can also be influenced by a wide variety of foods and medications. While high-fibre vegetables are more likely to promote bowel movements, starchy foods such as potatoes are more likely to cause constipation. Another factor is water intake; too little water can dry out the stool and make bowel movements less frequent.
Tips for better bowel movements
As you may have noticed up to this point, diet has a significant influence on intestinal flora. However, there are other factors that can positively influence your bowel movements. Here are four simple tips that Homed-IQ recommends to improve your bowel movements:
- Exercise regularly, as exercise helps your body with digestion.
- Drink enough water; ideally around 2 litres per day.
- Avoid foods and drinks known to irritate your stomach. These include alcohol and caffeine, as well as spicy and greasy food.
- Consume enough dietary fibre. This includes fruits and vegetables, legumes, and whole grain products)
References
Blake, M. R., Raker, J. M. & Whelan, K. (2016, 5. August). Validity and reliability of the Bristol Stool Form Scale in healthy adults and patients with diarrhoea-predominant irritable bowel syndrome. Wiley Online Library. Retrieved April 15, 2022, from https://onlinelibrary.wiley.com/doi/10.1111/apt.13746
Dimidi, E., Christodoulides, S., Fragkos, K. C., Scott, S. M. & Whelan, K. (2014). The effect of probiotics on functional constipation in adults: a systematic review and meta-analysis of randomized controlled trials. The American Journal of Clinical Nutrition, 100(4), 1075–1084. https://doi.org/10.3945/ajcn.114.089151
Lewis, S. J. & Heaton, K. W. (1997). Stool Form Scale as a Useful Guide to Intestinal Transit Time. Scandinavian Journal of Gastroenterology, 32(9), 920–924. https://doi.org/10.3109/00365529709011203
MedlinePlus. (2015, March 25). Bowel Movement. Retrieved April 15, 2022, from https://medlineplus.gov/bowelmovement.html
Miletic, B. (2021, 9. November). How often should you have a bowel movement per day? Futura Sciences. Retrieved on April 15, 2022, from https://www.futura-sciences.com/de/wie-oft-sollte-man-per-tag-stuhlgang-haben_7287/
Modi, R. M., Hinton, A., Pinkhas, D., Groce, R., Meyer, M. M., Balasubramanian, G., Levine, E. & Stanich, P. P. (2019). Implementation of a Defecation Posture Modification Device. Journal of Clinical Gastroenterology, 53(3), 216–219. https://doi.org/10.1097/mcg.0000000000001143
NIH. (2021, 5. Mai). Diarrhea. National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved April 15, 2022, from https://www.niddk.nih.gov/health-information/digestive-diseases/diarrhea/all-content




